GLP-1 Mechanism: More Than Just Weight Loss
GLP-1 (glucagon-like peptide-1) receptor agonists are medications that mimic a natural gut hormone. While famous for causing weight loss, their primary medical function is to control blood sugar. Their benefits extend far beyond the scale.
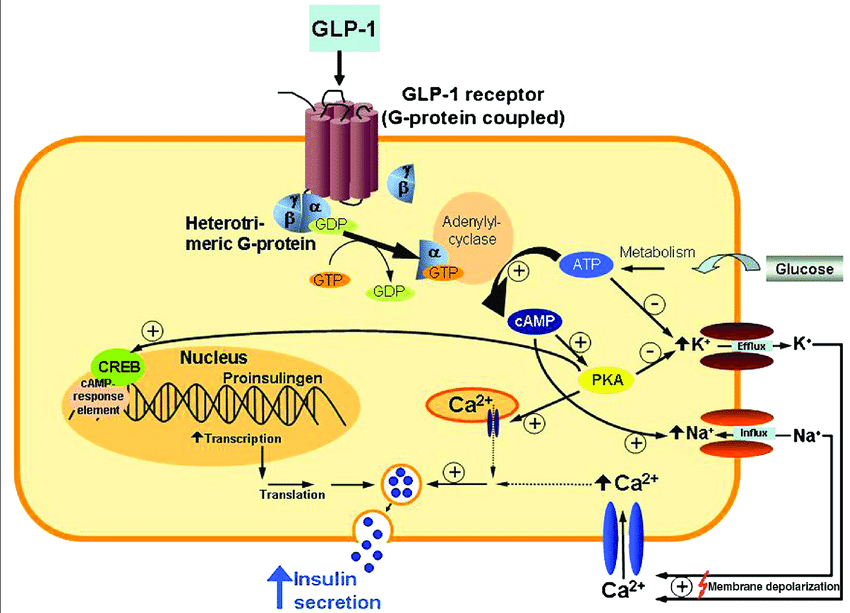
Blood Sugar Control (The Primary Goal):
-
- Stimulates Insulin: GLP-1 tells your pancreas to release insulin only when blood sugar is high (this is called a "glucose-dependent" mechanism, which reduces the risk of low blood sugar).
- Blocks Glucagon: It suppresses glucagon, a hormone that tells your liver to release stored sugar.
Weight Loss Mechanisms:
-
- Slows Digestion: It slows down how quickly food leaves your stomach (gastric emptying), making you feel full longer.
- Reduces Appetite: It acts on the appetite centers in your brain, reducing hunger and food cravings.
Wider Metabolic & Organ Benefits:
-
- Heart Protection: Studies show GLP-1 drugs significantly reduce the risk of major cardiovascular events like heart attacks and strokes. They can also help lower blood pressure and improve cholesterol levels.
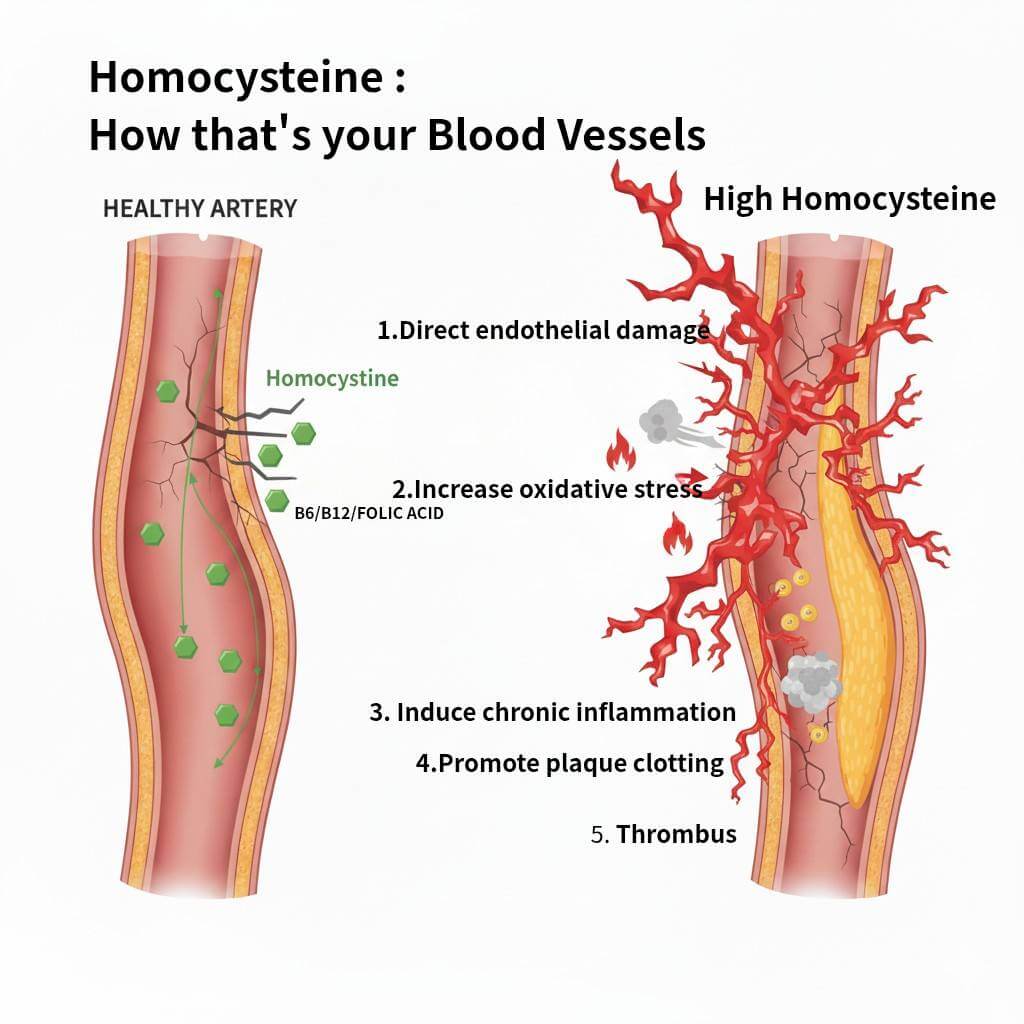
- Kidney Protection: They have a protective effect on the kidneys, slowing the progression of diabetic kidney disease.
- Liver Health: They can reduce fat buildup in the liver, helping to improve conditions like non-alcoholic fatty liver disease (NAFLD).
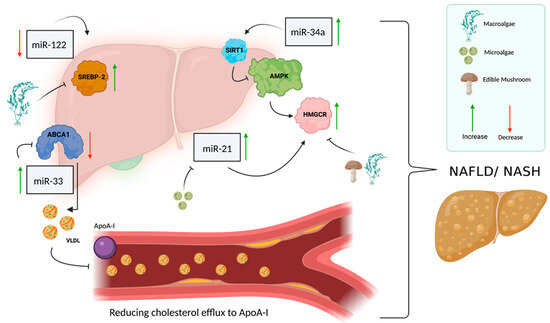
- Anti-Inflammatory: GLP-1 has a broad anti-inflammatory effect throughout the body, which is a key factor in its heart, kidney, and liver benefits.
Insulin Resistance & Metabolic Syndrome
These two conditions are deeply interconnected. Insulin resistance is a root cause, and metabolic syndrome is the clinical diagnosis of the resulting problems.
What is Insulin Resistance?
-
- Insulin is a hormone that acts like a key, unlocking your body's cells to let glucose (sugar) in for energy.
- Insulin Resistance means your cells (especially in your muscles, fat, and liver) stop responding properly to insulin's "key."
- Your pancreas tries to compensate by pumping out more and more insulin to force the cells to open. This leads to high insulin levels (hyperinsulinemia) and, eventually, high blood sugar.
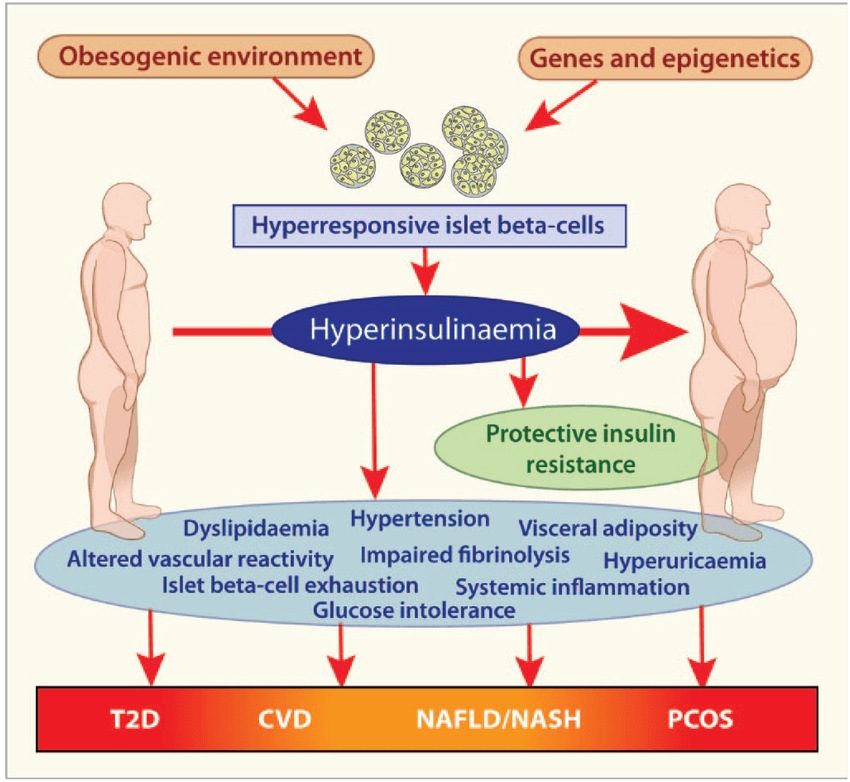
What is Metabolic Syndrome?
This is not a single disease, but a cluster of five risk factors. A diagnosis is made if you have at least three of the following:
-
-
- Abdominal Obesity: Excess fat around the waist (a high waist circumference).
- High Triglycerides: A type of fat in your blood.
- Low HDL ("Good") Cholesterol: The cholesterol that helps clear out the "bad" kind.
- High Blood Pressure (Hypertension):
- High Fasting Blood Sugar: A sign of prediabetes or diabetes.
- The Connection: Insulin resistance is the underlying driver for most of these conditions.
For example, high insulin levels can signal the liver to produce more triglycerides and can cause the kidneys to retain salt and water, raising blood pressure.
Cholesterol Myths: The Truth & Liver Function
Cholesterol is a waxy substance that is essential for building cells and making hormones. The idea that it's "all bad" is a common myth.
Myth 1: All cholesterol is bad.
-
- Fact: There are two main types. LDL (Low-Density Lipoprotein) is the "bad" cholesterol because it builds up in arteries. HDL (High-Density Lipoprotein) is the "good" cholesterol because it acts like a garbage truck, collecting excess cholesterol and taking it back to the liver to be removed.
Myth 2: Eating high-cholesterol foods (like eggs) is the main cause of high blood cholesterol.
-
- Fact: For most people, dietary cholesterol (what you eat) has a surprisingly small impact on your blood cholesterol. Your body makes its own! The much bigger dietary culprits for raising your "bad" LDL cholesterol are saturated fats (in red meat, butter, full-fat dairy) and trans fats (in many processed foods).
Myth 3: You can feel it if you have high cholesterol.
-
- Fact: High cholesterol has no symptoms. The only way to know your levels is through a blood test.
The Connection to Liver Function
The liver is the central processing plant for cholesterol.
- It MAKES Cholesterol: Your liver produces about 80% of the cholesterol in your body (endogenous cholesterol).
- It CLEARS Cholesterol: The liver is the only organ that can remove cholesterol from the body. It does this by converting it into bile acids, which are then excreted through digestion.
If your liver is damaged (for example, by fatty liver disease (NAFLD)), it can't do its job properly. This creates a vicious cycle:
- A damaged liver struggles to clear LDL cholesterol, so blood levels rise.
- High levels of fat and cholesterol in the blood can, in turn, cause more fat to be deposited in the liver, worsening the liver disease.
Keto vs. Mediterranean: Which is Better for Anti-Inflammation?
For most people, the Mediterranean diet is the superior and more sustainable choice for long-term anti-inflammation.
Mediterranean Diet:
-
- How it works: This diet is rich in foods that are naturally anti-inflammatory, such as olive oil, fatty fish (omega-3s), nuts, fruits, vegetables, and whole grains.
These foods provide a wide array of antioxidants and polyphenols that directly combat inflammation.
- Suitability: It is well-balanced, easy to maintain for life, and has extensive, long-term research supporting its benefits for heart health, brain health, and lowering inflammation.
Ketogenic (Keto) Diet:
-
- How it works: This very low-carb, high-fat diet fights inflammation through a different mechanism. By forcing the body into a state of ketosis (burning fat for fuel), it produces molecules called ketone bodies.
One of these, beta-hydroxybutyrate (BHB), has been shown to have potent anti-inflammatory effects.
- Suitability: Keto can be very effective for reducing inflammation, but it is extremely restrictive and difficult to sustain. A poorly constructed keto diet (high in saturated fats like butter and bacon, low in vegetables) can actually increase inflammation.
For anti-inflammatory benefits, it must be well-formulated with healthy fats, like a "Mediterranean-style" keto diet. It is often considered a short-term, therapeutic diet for specific conditions rather than a lifelong eating pattern.
Conclusion: While keto can be anti-inflammatory, the Mediterranean diet is the more suitable, balanced, and proven choice for general, long-term anti-inflammatory eating.
Why "Lean" People Get Fatty Liver
Fatty liver disease (NAFLD/MASLD) is not exclusively a disease of obesity. A "normal" Body Mass Index (BMI) can be dangerously misleading. Here’s why a lean person can develop it:
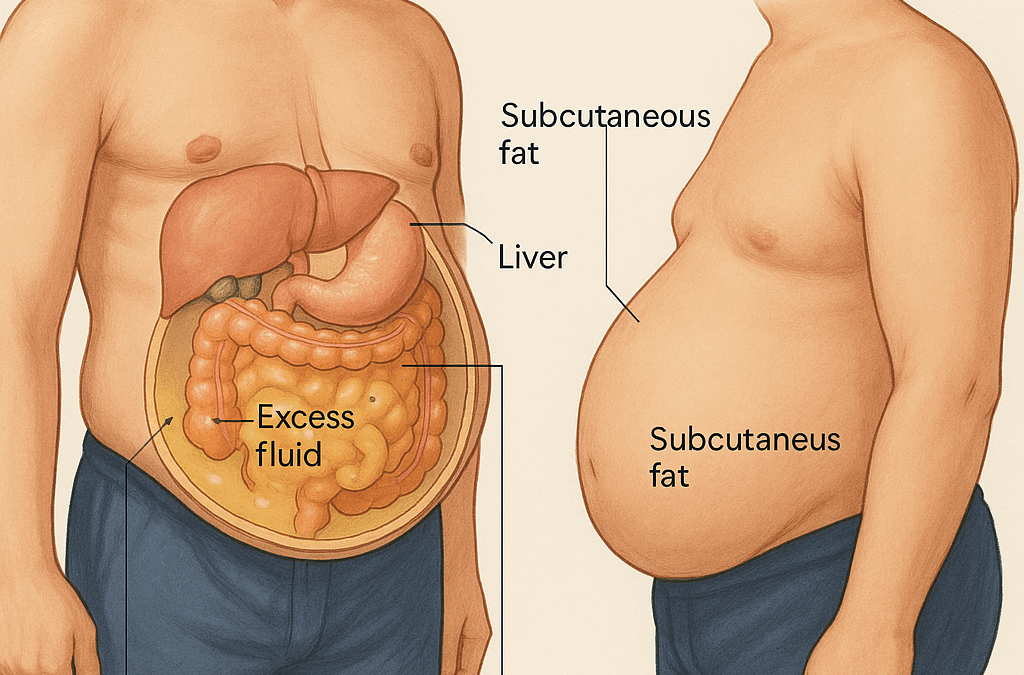
- Visceral Fat (The "Hidden" Fat): This is the most important reason. A person may have a low BMI but still carry a high amount of visceral fat, which is fat stored deep inside the belly, wrapped around organs like the liver, pancreas, and intestines.
This type of fat is metabolically active and highly inflammatory, pouring fatty acids and inflammatory signals directly into the liver.
- Genetic Predisposition: Genetics play a huge role. A specific gene variant, PNPLA3, is strongly linked to fatty liver.
People with this variant (which is more common in some ethnic groups) are much more likely to accumulate fat in their liver, even if they are not overweight or insulin resistant.
- Metabolic Dysfunction: A lean person can still be "metabolically unhealthy." They may have underlying insulin resistance, high triglycerides, and low HDL cholesterol—all classic risk factors for NAFLD.
- Diet: A diet high in fructose (especially from sugary drinks and processed foods) and refined carbohydrates is a powerful driver of de novo lipogenesis—a process where the liver turns excess sugar directly into fat.
This can happen even if total calorie intake isn't high enough to cause obesity.





